Negative pressure wound therapy (NPWT) is a popular treatment modality for the management of both acute and chronic wounds. NPWT systems (such as 3M™ V.A.C.® Therapy) promote wound healing by drawing wound edges together, removing infectious materials and exudate, and promoting the formation of granulation tissue. Orgill and Bayer described four primary effects of NPWT on wound healing: macro-deformation and wound contracture, stabilization of the wound environment, edema reduction and exudate removal, and micro-deformation leading to cellular proliferation on the wound surface.1 In 1997, Argenta et al. first published the use of foam dressings with negative pressure for promoting wound healing.2 Since then, this wound therapy modality has undergone several developmental changes and what is currently seen in clinical practice today is a remarkably advanced iteration of the very first NPWT devices.
Intrinsic and Extrinsic Factors Affect Wound Healing
There are numerous variables that affect wound healing biology. These variables include intrinsic factors specific to the wound itself as well as extrinsic host factors. Intrinsic wound factors need to be assessed and managed in order to promote wound healing. Wound debris and thick exudate need to be removed from the wound bed in order to promote the development of healthy granulation tissue. When managing bacterial bioburden, a variety of methods ranging from systemic antibiotic treatment, serial debridement, the use of wound dressings impregnated with antimicrobial agents, or wound cleansing can be employed. With respect to extrinsic host factors, variables that include systemic conditions are of importance, particularly in the case with diabetes and associated foot wounds. Uncontrolled high blood sugar as well as insensate feet clearly impact wound healing negatively. As part of the overall patient care, the assessment and management of comorbid conditions can help remove barriers to wound healing.
Negative Pressure Wound Therapy With Instillation and Dwell
3M™ Veraflo™ Therapy combines the benefits of V.A.C.® Therapy with automated topical wound solution instillation and removal. Veraflo Therapy can help facilitate wound management by providing contained and controlled wound cleansing via the instillation of topical wound cleansers and repeated V.A.C.® Therapy cycles that can help soften and loosen wound debris, delivering topical antiseptic wound solutions that can help manage bacterial bioburden, removing solublized wound debris and infectious materials during the negative pressure cycle, and promoting the formation of granulation tissue.3-7
Representative Veraflo Therapy Case Study
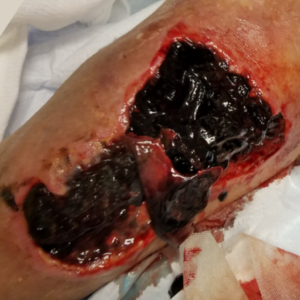
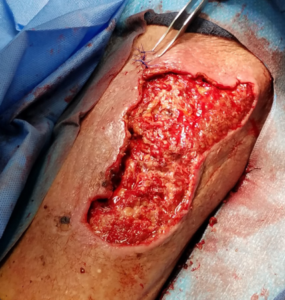
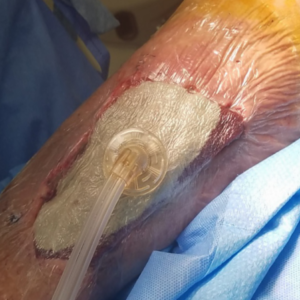
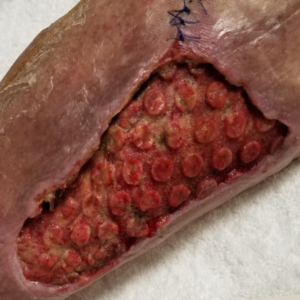
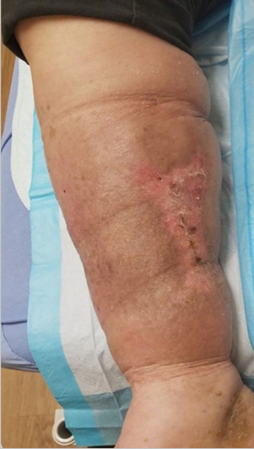
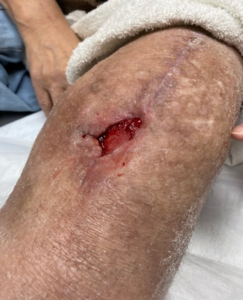
The following case study (adapted from Napolitano 20183) demonstrated the use of Veraflo Therapy in my practice. An 83-year-old male presented for care with a lower extremity wound following traumatic injury. Upon assessment, a large, gelatinous hematoma and extensive soft tissue necrosis involving about 80% of the right medial calf with compartment syndrome sequelae was noted (Figure 1). The patient underwent surgical debridement and pulsed lavage (Figure 2). Veraflo Therapy using 3M™ V.A.C. Veraflo Cleanse Choice™ Dressing was applied in the operating room. Normal saline (30 mL) was instilled into the wound bed with an 8 minute dwell time, followed by 3.5 hours of continuous negative pressure at -125 mmHg (Figure 3). Dressings were changed every 2-3 days. After 3 days of Veraflo Therapy with V.A.C. Veraflo Cleanse Choice Dressing, healthy granulation tissue was observed in the wound bed (Figure 4). Veraflo Therapy was continued for a total of 6 days, after which, the patient was discharged to a skilled nursing facility with V.A.C.® Therapy (continuous negative pressure at -125 mmHg, with dressing changes every 2-3 days). After 21 days of V.A.C.® Therapy, the wound was 100% covered with healthy granulation tissue and ready for a skin graft procedure (Figure 5). Epidermal skin grafting was performed, and the wound healed without complications (Figure 6).

A New Silicone-acrylic Hybrid Drape Option for Veraflo Therapy
It is well understood that for a NPWT therapy construct to positively affect wound healing, a “seal” between the wound, wound dressing and periwound is essential.8 This is of particular importance for Veraflo Therapy in order to effectively control fluid instillation and prevent periwound complications. Traditionally, an adhesive, acrylic drape has been used for both V.A.C.® Therapy and Veraflo Therapy constructs. Although this drape is very effective in seal creation and maintenance, patient complications may arise including sensitivities to the adhesive acrylic material, periwound maceration, and pain upon removal. Potential issues with the traditional drape for the clinician include challenging handling characteristics such as sticking to gloves, and the inability to reposition the drape once placed. Additionally, seal creation in certain anatomic regions can be difficult requiring “picture framing” techniques in which additional strips of drape are needed to create an effective seal.
3M™ Dermatac™ Drape, a proprietary silicone-acrylic hybrid drape that provides both clinical and operational benefits, was commercially released in 2019 as an accessory to specific NPWT systems (Figure 7). In early 2021, Dermatac Drape became commercially available in the US for use with Veraflo Therapy as well. Constructed with a precise combination of silicone and acrylic, Dermatac Drape affords both the patient and clinician distinct benefits compared to traditional acrylic drapes as demonstrated in several conference posters.9,10 Clinician advantages include improved ease of use, ability to improve the seal around complex anatomic areas, no significant adherence to clinician gloves, and overall significant decrease in application time.4 Dermatac Drape advantages for the patient may include reduced pain dressing change as well as a decrease in periwound irritation and dermatitis (Figure 8).
Recently, we have begun using the Dermatac Drape in place of the standard acrylic drape. Our initial experience found that the Dermatac Drape was able to create and maintain an adequate seal while allowing for easy repositioning after initial placement around anatomically difficult areas. The gentle adhesion allowed for increased patient comfort at dressing changes and throughout wear time. Based on our initial experiences, we intend on incorporating the use of Dermatac Drape with Veraflo Therapy in our wound care practice.

Conclusion
Advancements in V.A.C.® Therapy technologies have led to the development of Veraflo Therapy, which combines the advantages of negative pressure with automated cycles of wound cleansing. In complex wounds, the addition of wound cleansing can help with wound bed management and promote the development of healthy granulation tissue. While the traditional Veraflo Therapy construct included an adhesive, acrylic drape, used over the foam dressings and periwound skin to create a seal, a new drape option is available. The Dermatac Drape, a proprietary silicone-acrylic hybrid drape, offers easy seal creation, better patient tolerance, better drape handling characteristics, and decreased patient pain at dressing changes compared to the traditional acrylic drape. Combining Dermatac Drape with Veraflo Therapy affords the clinician and patient significant positive benefits. Although this combination of Dermatac Drape and Veraflo Therapy is still in its infancy, the advantages of its use are clear.
Patient data and images courtesy of Ralph J. Napolitano, Jr., DPM, CWSP, FACFAS
As with any case study the results and outcomes should not be interpreted as a guarantee or warranty of similar results. Individual results may vary depending on the patient’s circumstances and condition.
NOTE: Specific indications, contraindications, warmings, precautions and safety information exist for these products and therapies. Please consult a clinician and product instructions for use prior to application. Rx only.
© 2021 3M. All rights reserved. 3M and other marks shown are marks and/or registered marks. Unauthorized use prohibited. 3M marks used under license in Canada. All other marks are property of their respective owners.
PRA-PM-US-03207 (06/21)
References:
- Orgill DP, Bayer LR. Negative pressure wound therapy: past, present and future. Int Wound J. 2013;10(Suppl 1):15-19.
- Argenta LC, Morykwas MJ. Vacuum-assisted closure: a new method for wound control and treatment: clinical experience. Ann Plast Surg. 1997;38(6):563-576.
- Napolitano RJ, Jr. Treatment of Acute Compartment Syndrome Sequela of the Leg: A Case Report Demonstrating Negative Pressure Wound Therapy with Instillation and Dwell Utilizing a Novel Dressing and Serial Automated Suction Blister Epidermal Harvesting and Grafting. Cureus. 2018;10(10):e3443.
- Obst MA, Harrigan J, Wodash A, Bjurstrom S. Early-stage management of complex wounds using negative pressure wound therapy with instillation and a dressing with through holes. Wounds. 2019;31(5):E33-E36.
- Brinkert D, Ali M, Naud M, Maire N, Trial C, Teot L. Negative pressure wound therapy with saline instillation: 131 patient case series. Int Wound J. 2013;10(Suppl 1):56-60.
- Teot L, Boissiere F, Fluieraru S. Novel foam dressing using negative pressure wound therapy with instillation to remove thick exudate. Int Wound J. 2017;14(5):842-848.
- Gabriel A, Camardo M, O’Rorke E, Gold R, Kim PJ. Effects of Negative-Pressure Wound Therapy With Instillation versus Standard of Care in Multiple Wound Types: Systematic Literature Review and Meta-Analysis. Plast Reconstr Surg. 2021;147(1S-1):68S-76S.
- Napolitano RJ, Jr. Advances in Negative Pressure Wound Therapy Dressings: Sealing the deal with DERMATAC Drape. Dialogues in Wound Management. 2020:1-2. Published August 2020. Accessed March 21, 2021.
- Napolitano RJ, Jr. Early use of a novel acrylic-silicone hybrid drape with negative pressure wound therapy in lower extremity wounds. Paper presented at: Presented at SAWC Fall 2019, October 12-14, 2019, Las Vegas, NV; 10/2019, 2019.
- Kharkar P, Napolitano RJ, Jr., Lantis J, et al. Assessment of a Novel Drape Containing Acrylic and Silicone-based Adhesives When Using Negative Pressure Wound Therapy. Paper presented at: Presented at SAWC Fall 2019, October 12-14, 2019, Las Vegas, NV; 10/2019, 2019.